On November 2nd CMS released the MACRA final rule for 2018. It’s 1,653 pages long. If you haven’t had a chance to dig into it, here are a few things to think about. Also, if you’re interested in a deeper dive into MACRA – watch a recent webinar Navigating Cancer hosted.
Medicare Access and CHIP Reauthorization Act of 2015 – or MACRA for short – created the Quality Payment Program to replace the Sustainable Growth Rate (SGR), changing the way Medicare reimburses clinicians. Moving forward, clinicians must choose from one of two incentive programs:
- Merit-Based Incentive Payment System (MIPS) which streamlines multiple existing quality programs under one overarching program; or
- Advanced Payment Models (APMS) like the Oncology Care Model, which provides an opportunity to earn a greater payment for taking on more advanced models of care
In the oncology space most clinicians will be participating in the MIPS, which consolidates three programs into one:
- Physician Quality Reporting System (PQRS)
- Meaningful Use (MU)
- Value-based Payment Modifier (VBM) – the start of reimbursement based on value delivered
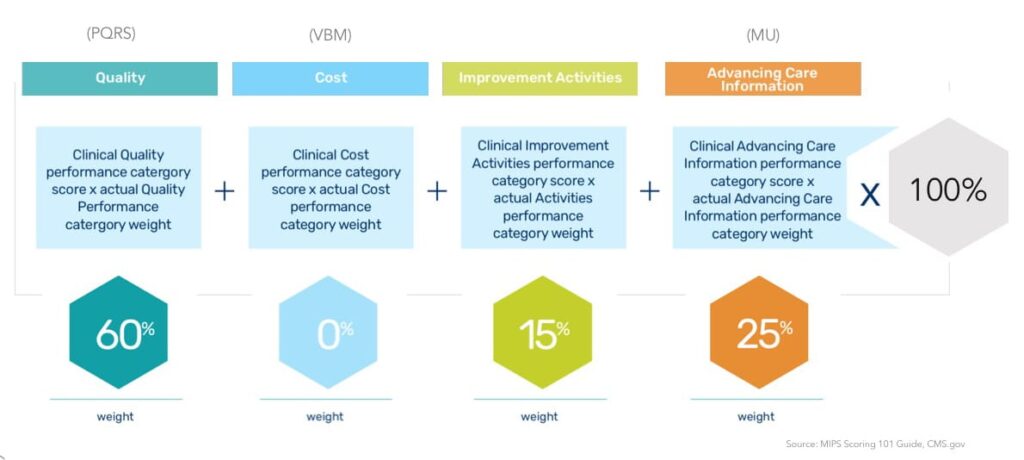
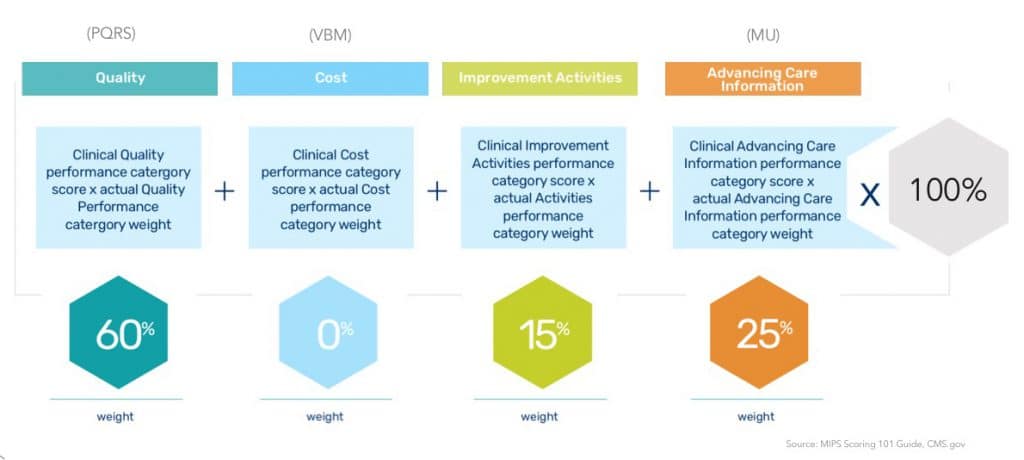
The MIPS performance categories today map roughly to those programs – Quality, Advancing Care Information, Cost – but now there is one additional category: Improvement Activities. This new category is intended to usher providers further along the value continuum and ensure they focus on care coordination, beneficiary engagement, and patient safety activities in addition to high quality, meaningful use of technology and lower costs.
Don’t underestimate the importance of starting early
Keep in mind with a two year claims lag, clinicians won’t really know if they’re on or off track until the first payment year in 2019. So the actions you take today will impact your reimbursement in the future. Start early putting the right processes and infrastructure in place to position yourself for success in 2019.
In addition to the uncertainty around your performance in the cost category, also keep in mind that payment adjustments will reach increasingly higher highs and lower lows. The SGR method resulted in minimal to zero adjustment to the Physician Fee Schedule (PFS) for the past 10 years and in these transition years before 2019, there is a +0.5%. Moving forward in 2019, the PFS will be based on individualized performance and could be hit with a 4% negative adjustment and up to a -5%, 7%, 9% adjustment in subsequent years.
What you can do to get ahead of the rest
Stakes are lower today, but they will increase rapidly in the next five years. Innovative oncology practices have already started participating in payer pilots that are similar to MIPS and have seen some early success. They have done a few things that enable them to proactively help patients get through treatment, prevent unnecessary hospitalizations and maximize the efficiency of their practices:
- Adding dedicated triage and symptom management pathways. This leads to quicker and more consistent intervention for patients to keep them on treatment.
- Prompting patients to report how they’re feeling on a regular basis. This enables the care team to know right away if a patient is experiencing a serious side effect and facing a barrier to medication adherence.
- Implementing patient relationship management software solution. Technology helps the care team manage and track it all – automate the delivery of information, view patient needs in order of severity, manage patients at a population level to ensure compliance in a value-based world.
For a deeper dive into how your MIPS composite score will be calculated, view a webinar.
Contact us at inquiries@navigatingcancer.com to learn more about the impacts of MACRA and how to prepare for success in value-based healthcare models.