Publications
Impact of remote symptom monitoring with electronic patient-reported outcomes on hospitalization, survival, and cost in community oncology practice: The Texas Two-Step Study
Using Navigating Cancer’s Health Tracker electronic patient reported outcome software, the Texas Two Step Study found a substantial impact on quality of care and associated costs for metastatic cancer patients:
- 39% Reduction in Hospitalization
- $1,146 decrease in monthly cost of care
- 83% of savings from reductions in inpatient and associated physician costs.
- 33% fewer adverse events (hospitalization, ER visits, and mortality)
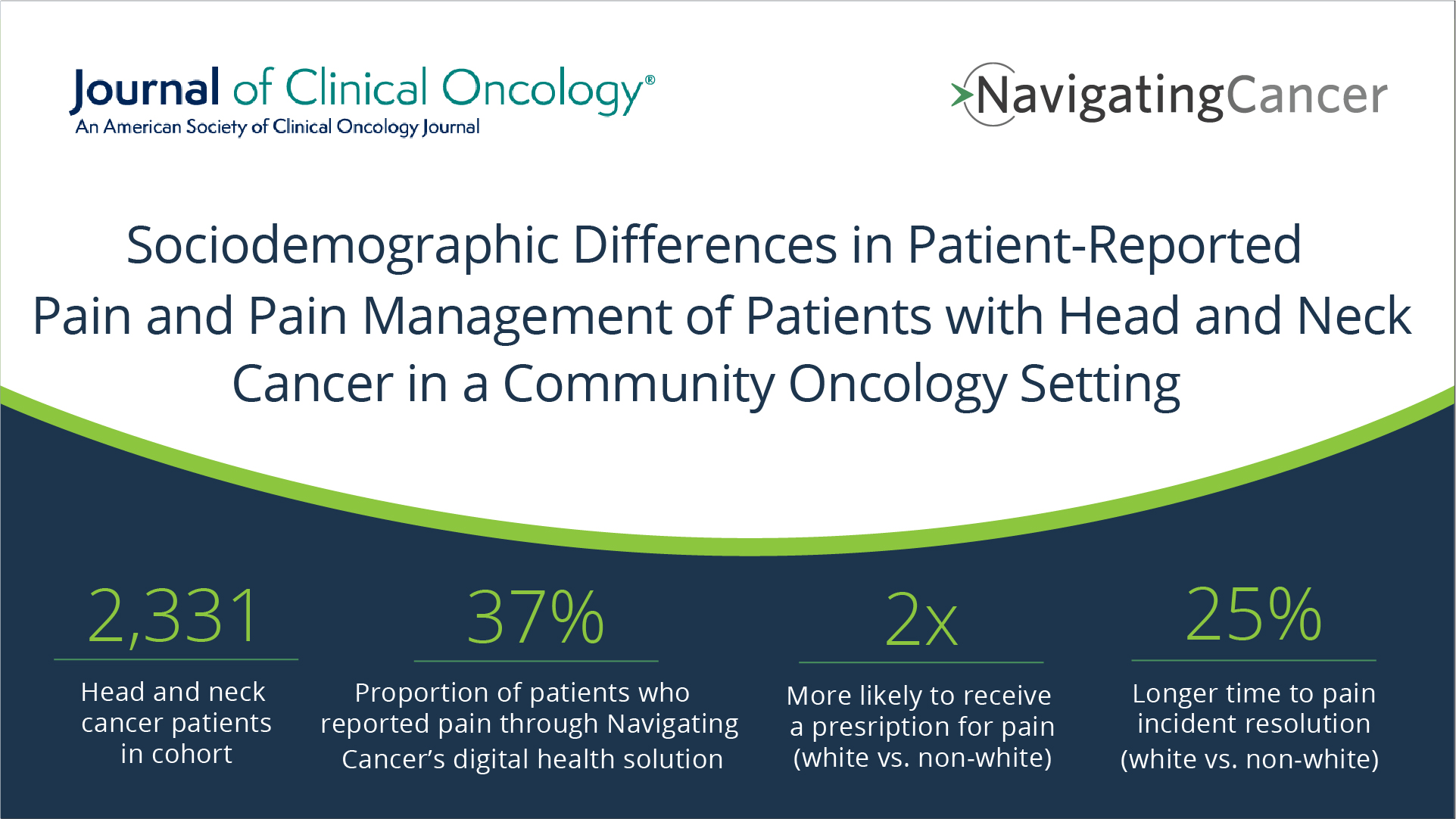
Sociodemographic Differences in Patient-Reported Pain and Pain Management of Patients With Head and Neck Cancer in a Community Oncology Setting
While there has been extensive research demonstrating racial disparities in pain reporting and management, this is, to our knowledge, the first published research leveraging oncology electronic patient-reported outcomes (ePROs) and nursing care management intervention data that further demonstrate disparities at the point-of-care.
Analyzing patient engagement with digital health tools to facilitate equity across a large statewide community oncology practice.
Digital health solutions can be used to support the cancer patient journey and we demonstrated high utilization in an array of sociodemographic variables in our population. However, tools designed and implemented with different populations in mind to reduce staff burden and lessen the digital divide should be further explored.
In collaboration with oncology clinics, cancer research institutes, and life science partners, we innovate in key areas to enable advancements in symptom management to improve patient outcomes.
Enhance clinical care through the development of products for cancer patients
Contribute to clinical research incorporating patient reported outcomes (PROs) data.
Power population health analytics for identifying at-risk patients and providing timely interventions.
Publications
Impact of remote symptom monitoring with electronic patient-reported outcomes on hospitalization, survival, and cost in community oncology practice: The Texas Two-Step Study
There is rising interest to implement electronic patient-reported outcomes (ePRO) for symptom monitoring to enhance quality of cancer care. Step 1 of the Texas Two-Step Study demonstrated successful implementation of an ePRO system in >200 sites of service of a large community oncology practice. We now report step 2 of this study which evaluates the impact of ePROs on outcomes among patients enrolled in CMS’ Oncology Care Model (OCM) program.
Debra Patt M.D., Ph.D., MBA
Sociodemographic Differences in Patient-Reported Pain and Pain Management of Patients With Head and Neck Cancer in a Community Oncology Setting
While there has been extensive research demonstrating racial disparities in pain reporting and management, this is, to our knowledge, the first published research leveraging oncology electronic patient-reported outcomes (ePROs) and nursing care management intervention data that further demonstrate disparities at the point-of-care.
Analyzing patient engagement with digital health tools to facilitate equity across a large statewide community oncology practice.
Digital health solutions (DHS) allow for enhanced remote communication between patients and clinical staff and the COVID-19 pandemic has brought these tools to the forefront of care delivery. Once adopted, barriers to adequate utilization still exist. Given the important need to decrease digital divides, and the diversity of patients and care settings across our clinic’s 220 sites of service, we sought to understand how utilization of oncology DHS may be limited among certain populations.
Debra A. Patt, Amila Meera Patel, Kathryn Elizabeth Hudson, Susan Marie Escudier, Holly Books, Sydney Townsend, Arun Bhardwaj, Bhanu Kaushik, Ben Pearson, Christopher Bays, Ethan Basch
Evaluating mass implementation of digital health solutions to improve quality and reduce disparities in a large multisite community oncology practice.
There is a priority to accelerate the delivery of digital health solutions (DHS) to provide patients with enhanced means for accessing care, but lack of understanding of their utility in certain populations. There are concerns that equitable adoption translate into disparities. We sought to implement a portfolio of DHS across a large practice and characterize engagement across populations to enhance clinical informatics solutions that support care delivery.
Amila Meera Patel, Arun Bhardwaj, Ethan Basch, Kathryn Elizabeth Hudson, Susan Marie Escudier, Holly Books, Bhanu Kaushik, Ben Pearson, Christopher Bays, Sydney Townsend, Debra A. Patt
Identifying ways to improve digital access among minority communities
Genentech and Navigating Cancer researchers analyzed data from more than 200K people living with cancer, found that most communities of color have limited access and online communication with oncologists on digital health platforms.
A collaboration with Texas Oncology to realize the benefits of ePROs: Dancing the Texas Two-Step through a global pandemic.
In a study of real-world ePRO implementation, Texas Oncology targeted cancer patients initiating systemic therapy to enroll in the Health Tracker ePRO digital monitoring program. The process included patient screening, introduction to the program, enrollment, initiation, observation, and intervention through the triage board workflow. There was a 65% ePRO compliance rate in the 4375 patients enrolled, as well as high participation rates among patients 65 years and older, those completing ePROs via text message, and patients on oral treatment.